Use of a condom or a dental dam can reduce the risk of HPV infection, but cannot fully protect one from HPV infection, because HPV can infect skin that remains uncovered during sexual activity.
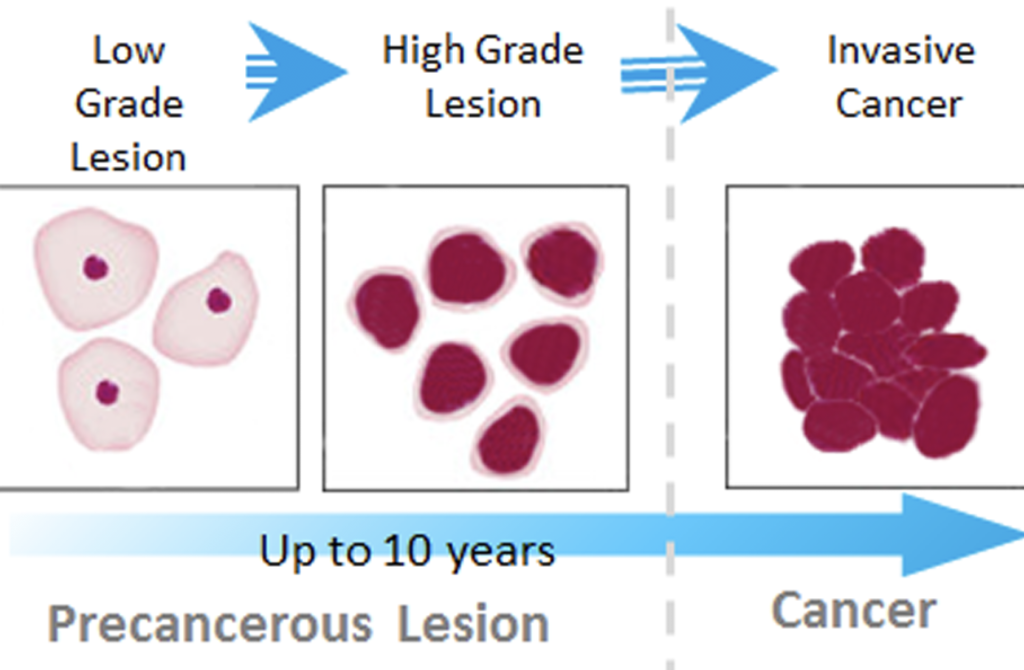
The best way to prevent HPV infection proactively is through an HPV vaccine–before a person becomes sexually active. The FDA-approved Gardasil covers four HPV types: HPV 6, 11, 16, and 18. HPV 6 and 11 are low-risk HPV types, and can cause genital warts; while HPV 16 and 18 are high-risk HPV types, and are responsible for 70% of cervical cancer cases. The HPV vaccine is highly effective in preventing HPV infection as well as the development of genital warts and cervical precancer lesions. However, HPV vaccine is prophylactic, thus it does not provide protection for individuals who are already exposed to HPV. The protection gained from the HPV vaccine is type-specific; it does not provide protection of infection of other HPV types besides these four HPV types.